Vietnam is in an early stage of implementing immune cell therapy in treating cancer patients, doctors say, as hope is high for more advances in the treatment approach after two scientists won this year’s Nobel in physiology or medicine for new discoveries in the area.
U.S. national James Allison and Japan’s Tasuku Honjo discovered how to harness the body’s immune system to fight cancer, for which they won the 2018 Nobel Prize in Physiology or Medicine announced on Monday by the Nobel committee at the Karolinska Institute in Stockholm.
The scientists’ groundbreaking work on the immune system has paved the way for a new class of cancer drugs that are already dramatically changing outcomes for patients, according to a press release by the committee.
In Vietnam, early steps are being taken to implement the breakthrough cancer therapy in hospitals with some promising results, according to doctors.
Prof. Dr. Ta Thanh Van, vice rector of Hanoi Medical University (HMU), said Vietnamese scientists have acquired the treatment approach from Japanese colleagues and are conducting their own research and tests on this new therapy to have it ready for clinical application.
“At first the Japanese side wanted to offer the treatment method for sale, but after some negotiation they agreed to have it transferred for free and only collect royalties when the therapy is officially applied in treatment,” Dr. Van said.
Van, who worked under Professor Tasuku Honjo during his fellowship in Japan between 1999 and 2003, said scientists at HMU’s Gene-Protein Research Center have received Ministry of Health’s permission to conduct a three-year scientific research, starting 2017, on the newly acquired cancer therapy.
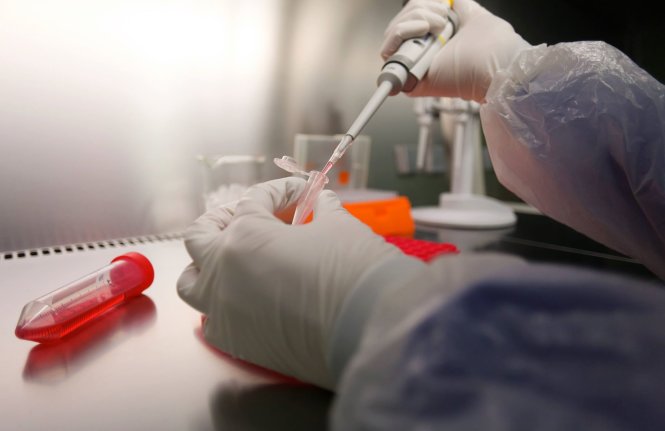
The study currently involves 70 patients diagnosed with five types of cancer who have their blood drawn for laboratory culturing of immune cells, which increase the cells’ number by many times.
The multiplied cells are then transferred back into the patients’ body via autotransfusion for six times in three months, Dr. Van said.
As of today, 15 cancer patients are undergoing this experimental treatment while hundreds are kept on waitlist, he added.
Assoc. Prof. Tran Huy Thinh, one of the researchers involved in the study, says he has noticed improvement in life quality among these patients, but more time is needed to determine whether the treatment is effective in reducing tumor size, prolonging the patient’s life or curing the disease.
The first transfusion of blood carrying lab-cultured immune cells only began in February this year, and eight months is not enough to adequately evaluate these parameters, he said.
Among their patients is one over 70 years of age who is diagnosed with late-stage gastrointestinal cancer and could barely move or do without painkillers before undergoing treatment.
“Since receiving the therapy, the patient has stopped taking painkillers and can now play with their grandchild for five hours each day,” Thinh said.
“The patient even recently traveled to southern parts of the country to visit relatives, which no one had thought would be possible before the treatment,” he added.
The biggest barrier between Vietnamese cancer patients and access to immunotherapy is probably the cost – a treatment cycle lasting one to two years can cost roughly VND120 million (US$5,100).
A full treatment regimen, consisting of 18 cycles, will set a patient back more than VND2.1 billion ($90,000) if they are not enrolled in a drug test, according to Dr. Le Tuan Anh, vice director of a cancer center at Cho Ray Hospital in Ho Chi Minh City.
Vietnam’s average yearly income per capita was VND53.5 million ($2,300) in 2017, according to a General Statistics Office report.
Despite some promising results, Prof. Dr. Andreas Beilhack from Germany’s Würzburg University Medical School believes we are still a long way from finding a cure-all therapy for the immensely varied group of diseases.
Even approved immunotherapy drugs only work on certain types of cancer, and even then only a minor percentage of patients using those drugs show signs of improvement, he explains.
For pulmonary and skin cancer, for example, the success rate is around 20-30 percent, Dr. Beilhack said.
While immunotherapy is typically considered safer than chemotherapy or radiotherapy as it harnesses the body’s own immune system to tackle cancer, there have been cases in human tests where the immune system overreacts, leading to life-threatening conditions, he added.
Nevertheless, patients in Vietnam have reasons to keep their hopes up that more lives will be saved thanks to these new discoveries in cancer treatments.
“Each new cancer therapy is invaluable, as it is another chance of survival for the patient,” said V., whose sister has been battling breast cancer for the last three years.
“Only those with cancer and their relatives can fathom this pain,” she said.
Like us on Facebook or follow us on Twitter to get the latest news about Vietnam!