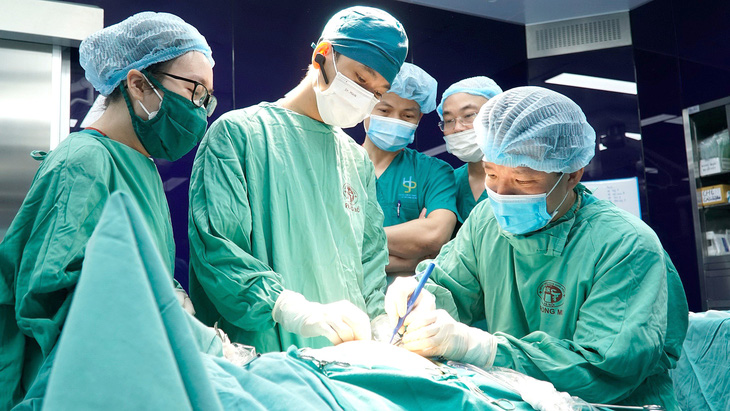
Editor’s note: In late November, an Australian patient sought laparoscopic surgery in Vietnam for a common bile duct cyst.
The procedure was conducted by Assoc. Professor Tran Ngoc Son, deputy director of Saint Paul General Hospital in Hanoi, who is among the few doctors specializing in single-hole laparoscopic surgery for choledochal cysts in pediatric patients in Vietnam.
Since 2011, Son has been a trailblazer as the first to perform single-hole laparoscopic surgery for common bile duct cysts in the country.
Over the years, he has successfully conducted over 300 surgeries using this technique, significantly alleviating pain and facilitating faster recovery for pediatric patients compared to conventional surgical methods.
Tuoi Tre (Youth) newspaper reporters recently interviewed Son to learn more about the technique.
Could you provide insights into the recent common bile duct cyst surgery conducted at the hospital for a foreign pediatric patient?
In late November, the family of an Australian patient revealed that their child had been unwell since October while residing in Indonesia.
There, they were informed by a doctor that open surgery could be conducted to remove their daughter’s common bile duct cyst.
Seeking alternative treatments, they discovered the single-hole laparoscopic surgery method for choledochal cysts.
Fortunately, a doctor in Bali, Indonesia, who had attended an international scientific conference, was familiar with this technique and provided the family with my contact information.
While initially exploring other options in hospitals in Australia and France, after more than a month, they decided to come to Vietnam for treatment.
The patient underwent a successful surgery using the single-hole laparoscopic method, with only a small scar left next to the navel, ensuring the baby’s esthetic appearance. Remarkably, just three days after the operation, the patient was already playing and showed rapid recovery.
How does this surgical technique offer advantages compared to other methods?
Traditionally, open surgery techniques were prevalent for common bile duct cysts, and many countries still employ this method.
However, in nations like Japan, the United States, Thailand, and Indonesia, single-hole laparoscopic surgery has become a standard for treating inguinal hernias in children.
In Vietnam, laparoscopic surgery is utilized to minimize trauma and ensure esthetic outcomes.
Although conventional laparoscopic surgery reduces trauma compared to open procedures, it typically involves making four incisions to place access ports for endoscopic instruments, potentially leaving three to four scars on the abdominal wall.
In contrast, the single-hole laparoscopic technique involves only one incision through the navel, with surgical instruments inserted and manipulated through this single small incision.
This method offers distinct esthetic advantages, as the patient will have no visible surgical scars since the navel serves as a natural scar that conceals the incision.
Additionally, recovery time is faster and the success rate of such surgeries is notably high.
|
|
| Assoc. Professor Tran Ngoc Son, deputy director of Saint Paul General Hospital in Hanoi. Photo: Duong Lieu / Tuoi Tre |
When did you first adopt this surgical technique? And why do you opt for a seemingly more challenging method compared to other techniques?
I first encountered the single-hole laparoscopic surgery technique through the navel announced by a doctor at an international scientific conference in Beijing, China in 2011.
Recognizing its numerous advantages, I believed it could be successfully implemented in Vietnam.
One notable feature of this technique is its compatibility with standard laparoscopic surgical instruments, eliminating the need for specialized tools.
Upon learning about it in 2011, I introduced this technique to pediatric patients.
Initially, the surgery duration was extended compared to conventional techniques, which typically take three to four hours for choledochal cyst surgery.
In my initial single-hole laparoscopic surgeries, the duration was five to six hours.
However, after approximately 10 surgeries, the duration gradually reduced, eventually matching that of other conventional techniques.
Despite its initial complexity, the technique offers various advantages, particularly in ensuring esthetics for patients, minimizing pain and facilitating faster recovery.
Motivated by the desire to provide the most effective treatment, I expanded the application of this technique to various surgeries, including inguinal hernia surgery, ovarian cystectomy, appendectomy, lymphatic cyst procedures, and other digestive defects.
Considering the higher incidence of congenital choledochal cysts in Vietnam and some other Southeast Asian countries compared to the global average, the application of this technique holds the potential to benefit a larger number of pediatric patients in the region.
Can this technique be transferred to lower-level hospitals, enhancing their capacity to treat patients?
This technique demands advanced technology and intricate surgical skills.
Unlike the conventional practice of making four incisions for laparoscopic instruments, this technique involves only one hole, making it more challenging.
The surgeon must possess advanced technical expertise to execute this method successfully.
An advantage of this approach is that it does not necessitate specialized laparoscopic surgical instruments or utilize other surgical tools.
Consequently, with a genuine commitment to study and enhance surgical techniques, doctors can feasibly explore and refine their proficiency in performing these surgeries.
Like us on Facebook or follow us on Twitter to get the latest news about Vietnam!